Rubella: A Comprehensive Guide to Symptoms, Contagion, and Management
Preventing Rubella Outbreaks The Importance of Vaccination
Introduction: Rubella, commonly known as German measles or 3-day measles, is a viral infection primarily affecting the skin and lymph nodes. While it often presents as a mild illness in children, it poses significant risks to pregnant women, potentially leading to severe health complications in their infants. The culprit behind rubella is the rubella virus, which is distinct from the measles virus and spreads through the inhalation of virus-infected fluid. Thanks to widespread immunization, the frequency of rubella epidemics, which used to occur every 6–9 years, has significantly decreased. These epidemics primarily impacted children aged 5 to 9, often leading to cases of congenital rubella. Let’s delve deeper into the signs and symptoms, contagious nature, preventive measures, and management of rubella.
Causes: Rubella is caused by the rubella virus, which is transmitted through respiratory droplets when an infected person coughs or sneezes. It is highly contagious and can spread even before symptoms appear.
Rubella Outbreaks:

Rubella outbreaks can occur when the virus spreads rapidly within a community or population. These outbreaks are more common in areas with lower vaccination rates. The virus is highly contagious and can be transmitted through respiratory droplets, making it easy for it to spread from person to person.
Symptoms:
Rubella typically commences with a mild fever lasting 1-2 days, accompanied by swollen and tender lymph nodes, typically located at the back of the neck or behind the ears. Shortly after, a rash appears on the face, gradually spreading downward. This rash is often the initial noticeable sign of illness and can resemble other viral rashes, presenting as pink or light red spots that may merge to form uniformly colored patches.
In adolescents and adults, additional symptoms may include headaches, loss of appetite, mild conjunctivitis (inflammation of the eyelid and eyeball linings), a stuffy or runny nose, swollen lymph nodes in other parts of the body, and pain and swelling in the joints. However, many individuals with rubella exhibit few or no symptoms. The rubella rash typically persists for 3 days, while swollen lymph nodes may last for a week or more, and joint pain can extend beyond 2 weeks. Children usually recover within 1 week, while adults may experience a longer recovery period.
New Vaccine Technologies: In recent years, advancements in vaccine technologies have contributed to more effective rubella prevention. These technologies have improved the formulation and delivery of rubella vaccines, enhancing their safety and efficacy.
Contagious Nature:
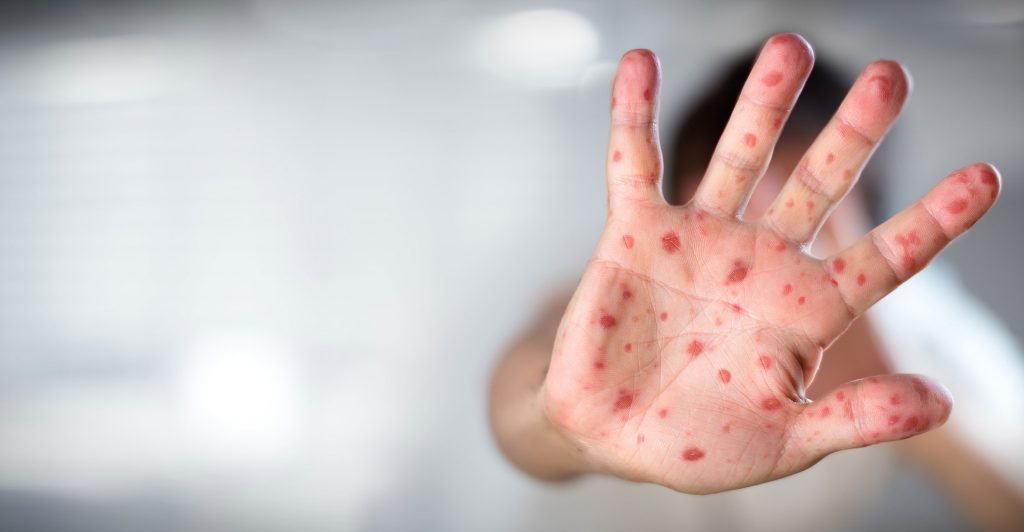
Rubella is highly contagious and primarily spreads through the transmission of virus-infected respiratory droplets via sneezing and coughing. Additionally, it can be transmitted through the sharing of food or beverages with an infected person. The most contagious period for individuals with rubella is 1 week before and 1 week after the rash appears. Notably, even individuals who are infected but asymptomatic can still transmit the virus.
Moreover, rubella can be transmitted from a pregnant woman’s bloodstream to her unborn child, potentially resulting in congenital rubella syndrome (CRS). Babies born with CRS face significant health risks, affecting their growth, cognitive development, heart, eyes, hearing, and organs such as the liver, spleen, and bone marrow. These infants can also shed the virus in their urine and respiratory secretions for an extended period, exposing those who are not immunized to the virus.
Prevention:
The most effective means of preventing rubella is through vaccination. Widespread immunization is essential to curb the virus’s transmission and safeguard infants from the severe health complications associated with congenital rubella syndrome.
In the current landscape, rubella infections are more prevalent among unvaccinated young adults than children. It’s noteworthy that approximately 10% of young adults lack the rubella vaccination, which could pose risks for future generations. Children typically receive the rubella vaccine at the age of 12–15 months as part of the standard measles-mumps-rubella (MMR) immunization or measles-mumps-rubella-varicella vaccine (MMRV). A follow-up dose is typically administered at 4-6 years of age. However, exceptions and special circumstances apply, such as early vaccination for children traveling abroad.
READ MORE ARTICLES Paiche The Enigmatic Giant of the Amazon Rainforest
Progress in Elimination Efforts: In Southeast Asia, vaccination programs have made significant progress, increasing regional coverage of rubella vaccination from 12% in 2013 to 86% in 2021. Case-based surveillance and laboratory networks have been established. Although rubella cases have decreased by 80%, challenges remain, including declining vaccination coverage during the COVID-19 pandemic.
The introduction of the rubella-containing vaccine (RCV) in Southeast Asia began in 2013, with Bhutan, the Maldives, Bangladesh, Thailand, and Sri Lanka being the initial countries to offer this vaccine. Over the course of 2013–2021, more countries in the Southeast Asia Region (SEAR) introduced the RCV. Prior to 2013, only three of these countries administered the second dose of the vaccine, while the rest adopted it between 2013 and 2021.
The WHO and UNICEF estimated that regional coverage of RCV was 12% in 2013, and it increased significantly to 86% by 2021. The highest coverage, reaching 93%, was recorded in 2019, before the onset of the COVID-19 pandemic. During the period from 2013 to 2021, supplementary immunization activities (SIAs) were conducted in all SEAR countries except Sri Lanka, benefiting over 514 million individuals.
Treatment
Rubella cannot be treated with antibiotics since they only combat bacterial infections, not viral ones. Typically, rubella resolves on its own without the need for medication unless it triggers additional complications.
Symptomatic Treatment: Doctors may recommend rest, plenty of fluids, and over-the-counter pain relievers like acetaminophen to reduce fever and discomfort. Isolation: Infected individuals should be isolated to prevent the spread of the virus, especially to pregnant women who are at high risk.
Vaccination:
Rubella can be prevented through vaccination. The measles, mumps, and rubella (MMR) vaccine is highly effective in preventing rubella. Routine vaccination is recommended, typically administered in two doses. Precautions: Vaccination: The most effective way to prevent rubella is through vaccination.
The MMR vaccine is typically given to children in two doses, one at 12-15 months and the second at 4-6 years of age. Immunity during Pregnancy: Pregnant women should ensure they are immune to rubella before becoming pregnant. If they are not immune, they should be vaccinated before conceiving because rubella can cause severe birth defects in the unborn child. Isolation: Infected individuals should be isolated to prevent the virus from spreading to others, especially to pregnant women. Isolation should continue for at least seven days after the rash appears.
1 Comment